DISCLAIMER: This article is not intended to promote or sell a product in any way, but rather to explain how research can be applied pragmatically towards the development of clinical rehabilitation technologies. The Scoliosis Traction Chair is not available for sale to the general public, or even to licensed Doctors of Chiropractic. It is only sold to doctors who are certified in the system of chiropractic scoliosis correction developed by the CLEAR Scoliosis Institute, and their patients.
Dr. Dennis Woggon, the founder of the CLEAR Scoliosis Institute, developed the concept of the Scoliosis Traction Chair (STC) in 2002, gradually refining it over the years. The idea behind the Scoliosis Traction Chair was straightforward; could it be possible to reverse a case of scoliosis into a “mirror-image” of itself, and find ways of keeping it there, without the use of a brace?
The concept of a chair was appealing for two main reasons. First, it removed the influence of the legs and lower extremities upon the patient’s posture, ensuring that the head, spine, and pelvis would be isolated and could be targeted more directly. Second, it still required the patient’s muscles in the neck and torso to react and engage to maintain an upright, stable position.
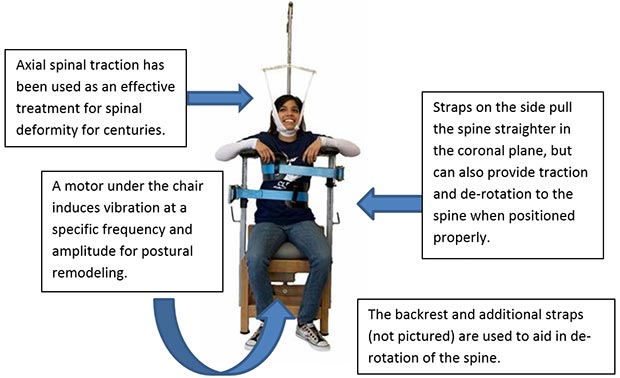
The armrests and back rest could be adjusted to influence the symmetry of the shoulders and the shoulder blades. If the right shoulder was higher than the left, for example, the left arm rest would be raised to reverse this. Similarly, the back rest could be positioned to induce positive de-rotation forces into the rib cage. Inclined seat cushions and wedges can be strategically placed to balance out the pelvis and influence the sacrum (tailbone), the foundation of the spine.
A low-force spinal traction component was incorporated into the chair which helps to relax the muscles by reducing their burden of supporting the head and neck, while helping to reduce forward head posture and restoring the natural alignment of the bones of the neck (the sagittal cervical lordosis).
Additional straps and belts were designed to pull the spine into a mirror-image configuration in the side-to-side (coronal) plane, while also de-rotating and uncoiling the spine in the top-down (axial) dimension.
Finally, whole-body vibration (WBV) therapy was added as a way of stimulating postural remodeling, enhancing muscle activation, and facilitating a more equal transfer of forces through the spinal column. While research on WBV therapy is still ongoing, there is some evidence to suggest that the specific frequency utilized by the STC (30 Hertz) can influence balance & co-ordination, reverse or prevent loss of bone density, engage muscles to contract more efficiently, and improve the health of the intervertebral discs.1-5
X-rays taken of patients in the Scoliosis Traction Chair demonstrate not only improvements in Cobb angle, but also in the rotation of the spine; in some cases, these results are superior to bracing.
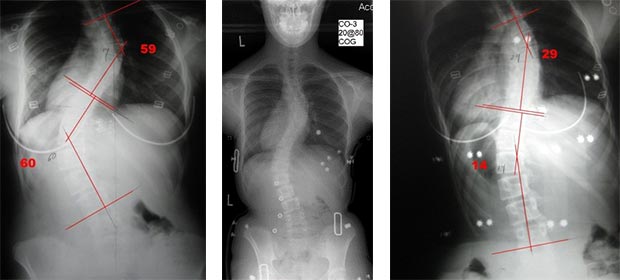
In the initial radiograph, the patient demonstrates a 59 degree thoracic Cobb angle and 22.5% rotation of the thoracic apical vertebra (T6), and a 60 degree Cobb angle with 24.5% rotation of the apical vertebra (L1).
In brace, the patient’s Cobb angles measure 55 and 49 (a 4 and 11 degree improvement respectively), and the rotation measures 35.1% and 29.5% (a 12.6% and 5.0% worsening respectively).
In the Scoliosis Traction Chair, the patient’s Cobb angles measure 29 and 14 degrees (a 30 and 46 degree improvement respectively), and the rotation measures 19% and 17.9% (a 3.5% and 6.6% improvement respectively).
The Scoliosis Traction Chair is only one part of the CLEAR Scoliosis Treatment Protocols. Each part of the treatment is intended to complement the others. In isolation, it is unlikely that any one therapy would be as effective as doing all of them together, and this applies to the Scoliosis Traction Chair as well. CLEAR does not recommend that the STC be used alone. CLEAR also requires that patients using the STC be under the care of a CLEAR certified doctor. Due to the customizable nature of the STC, a doctor using one who is not CLEAR certified will most likely end up making their patients worse, as shown by Stitzel et al.6
A patient’s first experience with being placed in the Scoliosis Traction Chair can be awkward at first – much like being placed into a scoliosis brace for the first time. However, STC therapy should not be painful; if it is, the set-up of the chair is probably wrong and needs to be re-done. Most patients have no problems being in the STC for 30 minutes, twice daily. Mild side effects from the vibration have been reported, including nausea and dizziness; however, these side effects are rare and tend to go away quickly after the first few treatments. Muscle soreness can occur as well, as with any physical rehabilitation technique that involves stretching the spine and soft tissues.
In 2001, a scientist at the State University of New York in Stony Brook received a grant from NASA to study how whole-body vibration (WBV) could be used to achieve therapeutic benefits to the musculoskeletal system.1 The outcome of his work soon led to a general craze about WBV therapy, with additional researchers at other universities branching off to study other aspects of WBV, and marketers developing numerous platforms designed to capitalize on the research suggesting WBV therapy as a potential intervention for osteoporosis and other common ailments.
When the initial studies on WBV began to be published - as is the case with most initial research forays into new technologies - at first the findings were only suggestive of the opportunities for further research. Many times important parameters of WBV therapy - such as the frequency, amplitude, and direction of the vibratory waveform – were not reported, or were described only vaguely. As the importance of these factors in achieving specific outcomes began to be realized, additional studies were performed to determine how changing one factor might influence the results.
WBV therapy was first studied for its effects on bone formation, joint flexibility, and muscle tone. As an inductive science, research cannot be counted upon to provide all of the answers. If something has not been researched yet, after all, there can be no relying upon research to prove or disprove its efficacy. Rather, common-sense and deductive reasoning (commonly known as logic) are required.
Doctors of chiropractic understand how stimulation of muscle spindles increases stimulation of the cerebellum and other areas in the brain responsible for postural control through the process of afferentation. Researchers trying to understand how WBV therapy increased bone density postulated that it could be because of increased stimulation of postural muscles; as these long, strong muscles contracted, they stimulated bone growth through adaptive responses.2,3 Using deductive reasoning, it was hypothesized that if WBV increased the activity of the muscles, it could also increase the rate of afferentation occurring between the brain and the postural muscles, and thus promote better balance, proprioception, and posture by increasing the rate at which the body and the brain communicate with each other. If this rate of communication is increased, postural rehabilitation exercises performed with the aid of WBV therapy should be more effective than exercises performed alone.
Problems with vestibular function, proprioceptive deficits, and issues with postural control have all been observed in patients with idiopathic scoliosis.4,5 These balance-related disorders are also common to another segment of the population; namely, people living with Parkinson’s disease. In a recent study investigating the effect of WBV therapy on improving balance & postural stability in patients with this condition, a significant benefit was found.6 Although the effect of WBV therapy on improving vestibular deficits in scoliosis patients has not been specifically investigated, it is logical to assume that it may be similarly effective.
The most common management strategy for idiopathic scoliosis is orthopedic bracing; one of the most common braces used in North America is the Boston brace, developed in the early 1970’s by Dr. John Hall and Mr. William Miller of the Boston’s Children’s Hospital. Unfortunately, the rate of scoliosis surgeries has been steadily increasing since the 1980’s, when this brace achieved common usage.7
The action of a rigid brace such as the Boston brace, or any inflexible orthosis, is quite simple: it restricts motion. Immobilization results in muscle atrophy and degeneration of synovial joints, including the intervertebral discs of the spine. At the University of Vermont, the biomechanicist Dr. Ian Stokes performed a series of animal experiments that clearly demonstrated when motion was inhibited at the level of the IVD, the structural rigidity of the spine increased.8 This has dramatic implications for scoliosis bracing; if bracing is applied in a case of early-onset scoliosis, and bracing inhibits spinal mobility, could the resultant disc degeneration actually contribute to the development of a permanent spinal deformity? This is a question worth raising, in line with primum non nocere.
A study conducted by the Department of Mechanical Engineering at L’Ecole Polytechnique in Montreal, Canada, suggests that the fundamental philosophy behind the application of bracing may be flawed. Examining the problem from a purely biomechanical point of view, the researchers at L’Ecole Polytechnique suggested that, in fact, the Boston brace might be more beneficial if the current design were reversed - to paraphrase, the results could be improved if the brace were worn backwards:
“Boston brace treatment produces complex trunk motions that tend to shift the spine and rib cage anteriorly, with little de-rotation and lateral displacement to the left, whereas ideal expected correction would be the opposite.”
“A more optimal way to achieve trunk corrections could be made by applying loads laterally on the convex side and on the anterior thoracic opposite the rib hump, with a system that constrains mechanically the posterior rib hump from moving backward.”9
When compressive forces are applied to the body, the instinctive reaction is for the body to resist against it. By wearing a brace for several hours out of each day, the body develops a neuromuscular pattern of continually resisting against the applied force. When the brace is removed, the rebound effect, combined with muscles weakened by atrophy, could actually lead to increased progression of the scoliotic curvature.
Considering how the body responds to compressive forces, perhaps a different mechanism could be applied to achieve better results; namely, tractive or pulling-type forces. Pulling, as opposed to pushing, is less readily resisted by the body, and thus works with the body rather than against it. Greater reduction of spinal deformity could potentially be achieved when the muscles are engaged to facilitate the improvement rather than fight against it or be immobilized by the external forces applied.
Another important aspect to consider regarding the scoliotic deformity is its three-dimensional nature. The very term “scoliosis” is misleading, as it implies a lateral curvature of the spine. While scoliosis may be commonly measured and diagnosed in this fashion (namely Cobb angle), the sagittal and axial planes are also involved and contribute to the etiopathogenesis and progression of this spinal disorder.10 For this reason, it is more appropriate to refer to the scoliotic spine as a ‘helix,’ rather than a curve.11 Bracing is fundamentally flawed, due to its inherent inability to address the spine in all three dimensions. CT and three-dimensional x-ray systems consistently show that, even in cases of bracing where the lateral deviation of the spine as measured by Cobb angle is reduced, there is a worsening of the sagittal balance and no effect on the axial vertebral rotation12 (which, through the attachment of the ribs, is primarily responsible for the cosmetic deformity that is considered to be pathognomonic for the disorder of scoliosis). A more effective system of spinal correction should be measured not only by its ability to reduce the deformity in the coronal plane, but also in the other two dimensions (high school experiences aside, most of the people we encounter in life are not one-dimensional).
The earliest systems of spinal instrumentation did not address the axial or sagittal planes; in fact, Harrington rods caused a worsening of sagittal balance.13 New methods do not focus purely on the correction of the spine in the coronal plane, and one of the reasons used to justify the higher cost of newer systems of spinal instrumentation is the improved three-dimensional correction they can achieve.14
It is interesting to note that axial spinal traction is the earliest described form of treatment for scoliosis, and its role in the management of scoliosis has been well-documented over the centuries,15 yet today spinal traction is seldom used in the management of scoliosis. At one point the Milwaukee brace (the precursor to the Boston brace) incorporated a cervical halter which aimed at providing axial traction to the spine, but it was discontinued due to its social unacceptability as well as its unfortunate side effect of inducing TMJ problems in brace wearers. Currently, traction is used in the orthopedic management of scoliosis only in a hospital setting; under general anesthesia to evaluate the flexibility of the spine prior to surgery, and hence predict the post-surgical prognosis; and, halo traction (pins drilled into the skull and attached to a pulley unit), used pre-operatively to increase the flexibility of the curve and thus the improvement achievable through surgery. The historical foundations & reported benefits of axial traction should not be ignored; the one universal constant acting on all of our spines is gravity. It is common knowledge that the height of an individual is decreased throughout the day, sometimes by as much as a half-inch, due to the effect of constant gravitational loadbearing upon the intervertebral discs. A three-dimensional system of scoliosis management must by its very nature involve axial traction; the only alternative, axial compression, is intrinsically opposed to good spinal health. If traction can be used to increase flexibility of the spine and enhance long-term outcomes, it deserves to reclaim its place in the conservative management of spinal deformity.
Combining these observations and building upon published research, a chair was created that incorporates whole-body vibration (to stimulate motor-sensory communication between the brain & body along the spinocerebellar tracts) along with lateral traction (to pull, rather than push, the spine towards the ideal), axial traction (to decrease spinal rigidity and facilitate reduction of the deformity in the other two planes), and de-rotation (focusing on unwinding a helix rather than straightening a curve) to treat scoliosis more comprehensively, in all three dimensions. In preliminary clinical trials, this new device appears to have greater result in reducing not only the lateral deviation as measured by Cobb angle, but also the de-rotation as measured by Nash and Moe.16

In the initial radiograph, the patient demonstrates a 59 degree thoracic Cobb angle and 22.5% rotation of the thoracic apical vertebra (T6), and a 60 degree Cobb angle with 24.5% rotation of the apical vertebra (L1).
In brace, the patient’s Cobb angles measure 55 and 49 (a 4 and 11 degree improvement respectively), and the rotation measures 35.1% and 29.5% (a 12.6% and 5.0% worsening respectively).
In the Scoliosis Traction Chair, the patient’s Cobb angles measure 29 and 14 degrees (a 30 and 46 degree improvement respectively), and the rotation measures 19% and 17.9% (a 3.5% and 6.6% improvement respectively).
A thorough understanding of current research & research methods is of invaluable benefit to the treating clinician. In addition to providing solid evidence about current treatment methods, it suggests opportunities for future innovations in spinal rehabilitation and wellness promotion strategies. The Scoliosis Traction Chair is an example of how research can be used to develop new clinical rehabilitation strategies.
CLEAR provides a unique and innovative way of understanding scoliosis. Sign up to receive facts and information you won’t find anywhere else.

Would it strenght the spine and put the spine back to normal
The Scoliosis Traction Chair is one part of a comprehensive program which is designed to improve posture, reduce muscle imbalances, and re-align the spine. Together with the exercises and other therapies, it can be very effective in strengthening the muscles along the spine. Once scoliosis has progressed to a certain level, while it may be possible to reduce and stabilize the curvatures, it is unlikely that the spine can return to being completely straight without resorting to spinal fusion surgery.
Is there a traction chair in canada and where?
The Scoliosis Traction Chair is available in Canada and around the world. However, to ensure patient safety and positive results, it is only available to patients under the care of a CLEAR-certified doctor. Visit the Find a Doctor page to locate the CLEAR doctor closest to you!
Where in canada I can get the chair
You can only obtain the Scoliosis Traction Chair if you are under the care of a CLEAR-certified Doctor. To find the CLEAR doctor closest to you, please visit the Find a Doctor page (https://clearscoliosis.wpengine.com/find-a-doctor/).
Hi, Where in South African can I get the chair?
The Scoliosis Traction Chair is available for purchase through your CLEAR Certified Doctor. It cannot be purchased except by patients who are under the care of a CLEAR chiropractor.
Is the chair a available in Sydney Australia?
The Scoliosis Traction Chair is only available to patients under the care of a CLEAR Certified Doctor. While we do not currently have any CLEAR Certified Doctors in Australia, you can travel to receive care, and the STC can be shipped to your home to be used once you have completed the two-week Intensive Care program. More information on what to do if there isn't a CLEAR Doctor in your area can be found here: https://clearscoliosis.wpengine.com/blog/no-clear-doctor-near-you/
Is scoliosis traction chair is available in Delhi lndia
The Scoliosis Traction Chair can be shipped anywhere in the world, but is only available to patients who are under the care of a CLEAR Certified Doctor.
I use an STC at my Clear certified chiropractor's. Can you tell me what the chair with motor attached weighs, as I am thinking about purchasing one for home use, for use with the adjustments by my chiropractor, and my maintenance exercise program. All, of course, under instruction and care of my Clear certified chiropractor. Also, besides weight, would you have the size or dimensions of the chair when put together, and is the electric motor configured with copper wiring or aluminum wiring?
The chair weighs approximately 134 lbs (61 kg), and measures around 34" tall by 24" square. For more information about the technical specifications of the Scoliosis Traction Chair, please reach out to Vibe For Health (www.VibeForHealth.com) at [email protected], or (866) 520-4270. Congratulations on taking your care plan to the next level!
I am interested in the chair to correct my wife's scoliosis. I am a chiropractor and the adjustments are not helping much now.
Hello, Dr. Wang,
We recommend you contact a CLEAR-certified doctor for an appointment for your wife in order to learn how to properly use the scoliosis traction chair. You can find the CLEAR doctor nearest you here.
sir, where can i get a traction chair for correction of scoliosis in india pl guide me. my no.7353118576
The Scoliosis Traction Chair can be shipped anywhere in the world, but is only available to patients who are under the care of a CLEAR Certified Doctor. You can search for the CLEAR doctor nearest you here.
Hi,
1. Does the patient need to keep using the STC for whole life Please?
2. How many hours needed to use the STC per day normally please?
3. How long would be take to delivery the STC to New Zealand after visiting a CLEAR doctor, in Singapore or Japan, please?
Many thanks,
Wei
Hi, Wei. Unfortunately, your questions are very case-specific and it's difficult to answer without having more information. It sounds like you have a CLEAR doctor that you are working with. They would be able to address your specifics.
In general, the STC does not have to be used your whole life.
Time of use is prescribed per case, as it's varied per each individual scenario.
As for delivery times, I'm not sure on this.
I'm sorry I couldn’t have more specific answers, but I suggest you direct them to your treating doctor.
Hello,
I have a chair. Would you buy it back from me?
[email protected]
Thanks!
Hi, Cathy,
CLEAR does not buy back chairs. We can, however, contact you if we hear of anyone looking to buy a chair.
Hello, what type of battery is used in the vibration unit of the scoliosis traction chair? Thank you
Hello Bai.
There is actually no battery connected to the scoliosis traction chair. It uses a motor and gets plugged into the wall.